Lymphatics Of The Neck. Part 3
Description
This section is from the book "Applied Anatomy: The Construction Of The Human Body", by Gwilym G. Davis. Also available from Amazon: Applied anatomy: The construction of the human body.
Lymphatics Of The Neck. Part 3
Postpharyngeal Nodes
In the retropharyngeal space, toward the sides, between the buccopharyngeal fascia in front and the prevertebral fascia behind are located one or two nodes (see buccopharyngeal fascia, page 153, and retropharyngeal abscess, page 156). They seem to be the starting point, sometimes, of retropharyngeal abscess. They do not appear to get enlarged and project into the pharynx as tumors, as might be expected, so that they are not subjected to any surgical procedures.
Operating For The Removal Of Enlarged Cervical Nodes
This operation may be one of the most serious in surgery. Sir Frederick Treves says: "An operation of this kind should not be undertaken unless the surgeon has perfect confidence in his practical knowledge of the anatomy of the neck. Scarcely an instance can be cited in the range of operative surgery where a knowledge of the structure and of relations is more essential than in these excisions." The main difficulties encountered are in the avoidance of nerves and the control of hemorrhage. Air may enter the veins and cause death, and the thoracic duct may be wounded. The latter accident sometimes results fatally. The difficulty of the operation will depend on the size and number of the nodes, their location, and the character of the inflammation or other changes they have undergone. In an early stage the nodes may be lying loose in the tissues and can be readily turned out when once exposed. Later they may be matted to the surrounding structures by inflammatory deposits and then their separation is a matter of difficulty and danger.
The skin incisions may be either longitudinal or more or less transverse. The longitudinal incisions are usually along either the anterior or posterior border of the sternomastoid muscle, or the anterior edge of the trapezius. The transverse incision may be either opposite the hyoid bone - when it may be prolonged around the angle of the jaw and up to the mastoid process and over the suboccipital glands, or above the clavicle. • ,
As the skin and superficial structures are cut and the deep fascia opened, the superficial veins will be cut, hence the first anatomical fact to be borne in mind is the probable location of the veins. The most important of these is the external jugular. The internal jugular below the hyoid bone lies under the sternomastoid muscle and therefore is protected until the deeper dissection is begun. The external jugular runs about in a line from the angle of the jaw to the middle of the posterior edge of the sternomastoid muscle and thence downward to about the middle of the clavicle. Therefore an incision along the posterior edge of the sternomastoid will divide it at about the middle of the muscle, and the surgeon should be prepared to guard against an undue loss of blood when it is cut. Opening into the external jugular posteriorly between the middle of the sternomastoid muscle and the clavicle below are the posterior jugular, the transverse cervical, and the suprascapular veins.
These latter open into the external jugular 1 or 2 cm. above the clavicle and are almost certain to be cut in operations in the supraclavicular fossa. An incision along the anterior edge of the sternomastoid low down will cut the anterior jugular vein a short distance above the sternum as it winds beneath the sternomastoid to empty into the external jugular. An incision along the anterior border of the sternomastoid from its middle up is bound to cause free hemorrhage. The external jugular behind the angle of the jaw communicates with the facial, which empties into the internal jugular; hence division of the external jugular at this point also drains the blood almost directly from the internal jugular. A carelessly deep incision may wound the internal jugular itself in the region posterior to the hyoid bone. The internal jugular is more superficial at this point than it is lower down. The temporo-maxillary and posterior auricular veins will also be cut behind the ramus of the jaw.
Not only are veins cut but also nerves. The middle of the posterior edge of the sternomastoid is the point of departure of several nerves. The. superficial cervical runs directly transversely inward toward the thyroid cartilage. The auricu-laris magnus goes up to the lobe of the ear, and the occipitalis minor follows the posterior edge of the muscle up to the occiput. These three nerves are nerves of sensation and if they are divided only a certain amount of temporary anaesthesia will be produced over the parts they supply, hence their division is not a matter of much moment. The auricularis magnus is the largest of the three. The descending branches of the cervical plexus, which leave the posterior edge of the sternomastoid muscle immediately below the nerves just mentioned, proceed down under the deep fascia and will be seen only in a deeper dissection. The nerve which it is absolutely important to avoid is the spinal accessory. This enters the sternomastoid muscle on its under surface some little distance back of its anterior edge and 3 to 5 cm. below the mastoid process. It sends a branch to the muscle and leaves its posterior edge about its middle. It then passes downward and outward across the posterior cervical triangle under the deep fascia to enter the deep surface of the trapezius. If this nerve is divided, paralysis of the trapezius will certainly follow and as it is a motor nerve the shoulder of that side will drop considerably. This will be a permanent deformity because motor nerves do not seem to have their functions restored by time as so usually occurs when the nerves of sensation are divided.
If the nodes to be removed are superficial ones there are no other structures to be feared and the operation will be an easy one. If they lie deeper, then the sheath of the sternomastoid muscle is to be divided and the muscle pulled outward. Just above the level of the cricoid cartilage a small artery, the sternomastoid branch of the superior thyroid, enters the muscle and it will be divided. As the sternomastoid is raised and pulled outward care must be taken to avoid wounding the spinal accessory nerve. As this nerve enters the muscle from 3 to 5 cm. below the mastoid process and some distance back from the edge of the muscle, if it is necessary to divide the muscle it is best done high up above the entrance of the nerve, or low down. By so doing the nerve supply (from the spinal accessory) and blood supply are not interfered with and the function of the muscle is not so much impaired as it would be if divided near the middle. The nodes not only possess their own capsule but also a covering from the connective tissue in which they lie. Therefore to remove them they must be detached and separated from it usually by blunt dissection. When these strands of fibrous tissue from the nodes to the surrounding parts are strong they have to be caught with forceps and cut. They are to be clamped, to avoid possible bleeding. When the angle of the jaw is reached the communicating branch between the facial and external jugular veins must be clamped and cut. The parotid gland is to be pulled upward and inward. The nodes may stick to the jugular vein and carotid artery. The vein is on the outside and is likely to be the first encountered. When distended it overlies the artery. If collapsed its presence may not be suspected. Feel for the pulsation of the carotid artery and avoid the structure just to its outer side. The jugular vein may be so involved in the mass as to necessitate its removal. In such a case remember that posteriorly between it and the carotid artery is the pneumogastric nerve.
The sympathetic nerve lies deeper in the fascia toward its posterior surface and is not so likely to be wounded. Its superior cervical ganglion lies opposite the second and third vertebrae. Working still higher, the transverse process of the atlas or first cervical vertebra will be felt and seen below and to the inner side of the mastoid process. The connective tissue adherent to the nodes is attached to this transverse process and may have to be cut loose or scraped away. In doing so keep to the outer edge because the jugular vein and internal carotid artery lie on its anterior surface.
Beneath the sternomastoid runs the anterior scalene muscle and on it, coming from the third, fourth, and fifth cervical nerves, is the phrenic nerve; so that it is not permitted to dig into and disturb the muscular mass to the outer side of the common carotid artery on which these nodes frequently lie.
In operating in the submental region there is nothing to fear. The space between the two anterior bellies of the digastric muscles on the sides, the hyoid bone below, and down to the anterior surface of the mylohyoid muscle beneath, can be cleared out with impunity.
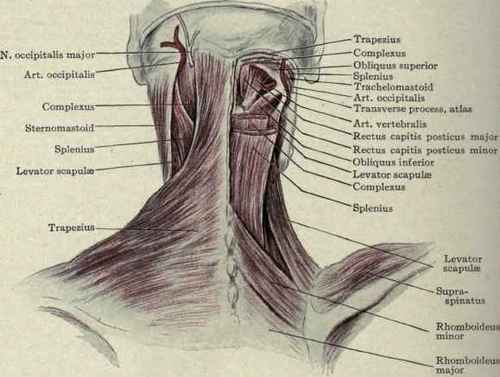
Fig. 182. - Superficial and deep structures of the back of the neck, showing the suboccipital triangle, formed by the rectus capitis posticus major, obliquus superior and obliquus inferior: the suboccipital nerve emerges from just beneath the art. vertebralis.
In the submaxillary region remember that the fascia covering the submaxillary gland is thin, so that the gland will probably be exposed as soon as the superficial structures are raised. As the facial artery and vein cross the mandible just in front of the masseter muscle, the vein is posterior. The artery goes under the gland and is adherent to it, so that as the gland is raised the artery is brought up also. The facial and lingual veins usually empty into the internal jugular, but, as shown in Fig. 168, they may receive a communicating branch from the external jugular and the anterior jugular and continue down as the anterior jugular to empty into the external jugular low down in the neck, beneath the sternomastoid muscle. The hypoglossal nerve will be seen lying on the hyoglossus muscle, but it is readily avoided. The lingual artery is beneath the hyoglossus muscle anteriorly but both it and the facial must be looked for as one nears the posterior belly of the digastric.
In the lower cervical region, opposite the cricoid cartilage, the omohyoid muscle will be met. It will sometimes be necessary to divide it. The sternohyoid and sternothyroid muscles and the thyroid gland are to be drawn inward and the sternomastoid outward. One should always keep away from the thyroid gland, as the recurrent laryngeal nerve runs behind it and on the oesophagus near the trachea. Cutting it will probably cause a permanent alteration in the voice. If the internal jugular vein has been removed, as it may be on one side, but not on both, beneath it one is liable to encounter the inferior thyroid artery below Chassaignac's tubercle on the sixth cervical vertebra, and further out the phrenic nerve on the scalenus anticus muscle, and lower down the transverse cervical and suprascapular arteries. The inferior thyroid veins usually run downward to empty into the innominate veins, but the lower portion of the anterior jugular vein and the middle thyroid veins will probably have to be ligated. The course of the various veins is quite irregular and large venous branches may be encountered at any place.
In the posterior cervical triangle the spinal accessory nerve must be avoided as it runs down and back from the middle of the posterior edge of the sternomastoid muscle. The external jugular, posterior jugular, transverse cervical, and suprascapular veins may all require ligation. Beneath the deep fascia (superficial layer) are the descending or supraclavicular branches of the cervical plexus from the third and fourth cervical nerves. Care should be taken not to mistake them for the spinal accessory nerve. If the nerve has been divided it should be sutured together again at the completion of the operation. It is hardly necessary to caution against wounding the subclavian vein; it is in front of the anterior scalene muscle. The artery is behind the muscle. Do not dig under it. It rests on the pleura, a wound or tear of which may mean a septic pleurisy and death. In the angle formed by the junction of the internal jugular vein and subclavian on the left side is the thoracic duct. If wounded death may ensue through persistent leakage of lymph, but not infrequently healing eventually occurs. Wounding of the corresponding lymphatic duct on the right side is not considered so serious, the chyle being carried by the left duct. The cords of the brachial plexus run down and across the posterior cervical triangle above the subclavian artery, but a little care will enable one to avoid them. This is one of the regions of the body in which exact surgery is essential.
Continue to:


