The Pelvis. Part 3
Description
This section is from the book "Applied Anatomy: The Construction Of The Human Body", by Gwilym G. Davis. Also available from Amazon: Applied anatomy: The construction of the human body.
The Pelvis. Part 3
Prolapse
The rectum and vagina as they pierce the pelvic floor may prolapse or protrude through the anus or vulva. Prolapse of the rectum is a common affection and if marked may drag down the peritoneum so that some coils of small intestine may be around the prolapsed part. In childbirth the pelvic outlet is frequently torn and the vagina prolapses and may drag the uterus down with it, or, the support being lost, the uterus descends and drags the vagina with it and everts it. The vaginal outlet, if much relaxed, allows the rectum to bulge downward and forward, forming a rectocele, or the bladder may bulge downward and backward, forming a cystocele (see Fig. 466, page 463).

Fig. 442. - Levator ani muscle and interior of pelvis; the bladder, uterus and vagina, and rectum have been loosened and turned down.
The Pelvic Fasciae
As the iliac fascia passes over the brim of the pelvis it covers the internal obturator muscle on the walls of the pelvis, hence it is called the obturator fascia. From the upper posterior surface of the arch of the pubes anteriorly to the spine of the ischium posteriorly this obturator fascia is thickened, forming the "white line" to give origin to the levator ani muscle. At the white line the obturator fascia gives off a visceral layer - the rectovesical fascia - which covers the inner or upper surface of the levator ani, then a second layer, the anal fascia, covering the under or outer surface of the levator ani muscle, while the obturator fascia itself is continued down on the obturator internus muscle to form the outer wall of the ischiorectal space. The rectovesical fascia passes downward and inward over the levator ani muscle to cover the pyriformis and coccygeus muscles behind, then the rectum, vagina, and bladder in front. In the male it covers the prostate gland, forming its sheath, and at its anterior portion forms the deep or posterior layer of the triangular ligament of the perineum. This pelvic fascia acts as a barrier between the abdominal and pelvic cavities above and the perineal region below. Pus originating above it tends to form an abscess which rises toward the abdominal cavity, and pus originating below it tends to work toward the surface in the perineum.
Iliac Vessels
The iliac arteries commence at the bifurcation of the aorta on the left side of the disk between the third and fourth lumbar vertebrae. This is 2 cm. (3/4 in.) below and to the left of the umbilicus and on a level with a line joining the highest points of the iliac crests. They run in a line drawn from this point to midway between the anterior superior spine of the ilium and the symphysis pubis. This is to the inner side of the middle of Poupart's ligament. They are about 15 cm. (6 in.) in length, the upper third, 5 cm. (2 in.), being the common iliac and the lower two-thirds, 10 cm. (4 in.), being the external iliac arteries. The internal iliac comes off opposite the sacro-iliac joint on or a little above a line joining the anterior superior spines. The right common iliac artery is a little the longer because it comes from the left side of the vertebral column, and the left common iliac vein is the longer because it goes to the right side. The left iliac veins lie to the inner side of the left iliac arteries in their entire course. The right iliac vein starts at the inner side of the right external iliac artery and then passes behind it to reach the vena cava on the right side of the vertebral column. The ureters cross the iliac arteries at their bifurcation, and in the female are accompanied by the ovarian arteries and veins. The genitocrural nerve passes downward on the external iliac artery and goes with it beneath Poupart's ligament. Lymphatic nodes accompany the iliac vessels and drain the lower extremity, the abdomen below the umbilicus and the pelvic viscera.
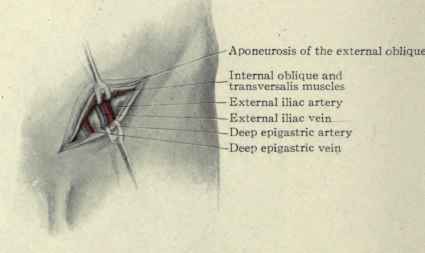
Fig. 443. - Ligation of the external iliac artery.
Continue to:


