Chapter IV. Dysentery
Description
This section is from the book "Diseases Of The Intestines", by Max Einhorn. Also available from Amazon: Diseases Of The Intestines A Text-Book For Practitioners And Students Of Medicine.
Chapter IV. Dysentery
Synonyms
Enteritis crouposa et necrotica; Amoebic dysentery.
Definition
An infectious disease characterized by specific ulcerations of the large intestine, giving rise to frequent bloody, mucous, or purulent dejections accompanied by tenesmus and general symptoms.
Etiology
Dysentery occurs under three different conditions: (1) As a disease principally during the warm season in temperate climates, appearing in local epidemics; (2) endemic in hot climates; (3) epidemic at certain times in all latitudes, being quickly disseminated, and also sporadic. While the endemic zone of dysentery is limited to places lying south of the fortieth degree of latitude, epidemics of the disease have occurred in almost every part of the globe. Dysentery is one of the oldest diseases known.' It was observed by Hippocrates and well described by Are-tseus and Celsus. Aretseus already recognized the ulceration of the intestines in dysentery.
Various causes have been adduced to explain the origin of the disease, and meteorological influences have been held responsible for its prevalence in local epidemics. The endemic dysentery of the tropics was generally ascribed to the combined action of heat and of the miasm of swamps. Sudden exposure to cold, eating of bad and spoiled food, and the use of stagnant or marshy water were all believed to be factors in producing dysentery. It is only within recent years that its infectious and also contagious character has been recognized. Sodre 1 says: "A careful etiological study shows that dysentery in whatever latitude it be observed is always due to the action of the same exciting cause, that it starts and is propagated always under the influence of infection and contagion, and that it should be included in the group of parasitic diseases." The exciting cause of dysentery often lies in the soil, in circumscribed foci of infection. These foci are represented by marshes and bogs which receive the drainage from dung heaps and cesspools, or by a soil impregnated with human dejections.
The contagious character of dysentery is best shown by the following report of Dr. Beauchef.2 This writer states that the French ship Loreit, anchored on the west coast of Africa, was in the best possible sanitary condition, not one of the crew being ill. She was then ordered to transport to Gorea the sailors of the sloop of war Eagle, among whom were twenty-nine dysenteric patients. A few days afterward, while on the high sea, dysentery spread among the crew of the Loreit and ceased only after all the patients had been landed at Gorea.
Among the causes which contribute to diffuse the dysenteric contagion and to produce the disease in an epidemic form the following may be mentioned: Crowding together of individuals, the vicissitudes of war, bodily privation, chiefly hunger. These factors are frequently found associated in times of war when epidemics of dysentery have often appeared, causing great ravages.
Since bacteria have been found to play an important part in the etiology of infectious diseases, many investigators have tried to discover the particular micro-organism producing dysentery. Various bacilli and cocci have been described and he)d responsible as etiological factors, but their relative significance has not been determined. As early as 1859, however, Lambl 1 called attention to the presence of amoebae in the intestinal contents. He found them in the stools of a child suffering from dysentery. Loesch,2 in 1875, observed amoebae in the dejecta of a patient suffering from chronic dysentery. He was the first to attribute the disease to this micro-organism. He also succeeded in experimentally producing a dysentery-like disease in a dog to which he had administered rectal injections of fecal matter containing amoebae. The observations of Loesch have been confirmed by Koch,3 who, while investigating dysentery in Egypt, found in post-mortem examinations numerous amoebae in the intestine at the base of the ulcers. The next important contribution on this subject was made by Kartulis,4 who, while practising in Alexandria, had an opportunity to observe several hundreds of cases of dysentery.
In more than five hundred post-mortem examinations he found the amoebae constantly in the faeces and on the surface of the ulcers, and in the abscesses of the intestine as well as of the liver. In other affections of the intestines Kartulis failed to detect the amoebae parasites. He also succeeded in cultivating them in infusions of sterilized dry straw, and twice produced dysentery in cats by inoculation with these cultures. Kartulis, therefore, declared the amoebae to be the true etiological factor of dysentery.
1 A. Sodre: " Dysentery, " Twentieth Century Practice of Medicine, vol. xvi., p. 241. 2 Beauchef . Cited after Sodre, loc. cit.
1 Lambl: " Beobachtungen und Studien aus dem Franz-Josef-Kinder-Spital, " 1860.
2 Loesch: "Massenhafte Entwickelung von Amoeben im Dickdarm. " Virch. Arch , Bd. lxv.
3 Koch: Cited after Sodre, loc. cit.
4 Kartulis: "Zur Aetiologie der Dysenterie in Aegypten. " Virch. Arch., Bd. 105. 1885.
Very soon afterward observations of a similar character were made both abroad and here. Thus Quincke and Roos,1 Hlava,2 Massaiutin,3 Nasse,4 and others abroad, and Osier,5 Stengel,6 Musser,7 Eichberg,8 Stockton,9 Councilman and Lafleur,10 and Harris 11 of this country have also described cases of dysentery with the presence of the amoebae parasites.
The theory of the amoebic origin of dysentery has been disputed by some writers, for they have found this micro-organism in the faeces in other intestinal disorders and, in some instances, even in the stools of healthy persons. Thus Schuberg 12 says: "The abundance of amoebae in dysentery is the effect and not the cause of the disease, the ulcerative lesions affording this habitual denizen of the intestines more favorable conditions for its development." The consensus of opinion, however, is that while harmless amoebae may occur in the intestinal tract, there exists a pathogenic variety of this organism which is specific for dysentery. For this reason Councilman and Lafleur proposed the name of amoebae dysenteriae for this special variety. The presence of the amoebae in the contents of abscesses of the liver, which are so often met with in dysentery according to Sodre, constitutes a powerful argument in favor of the amoebic etiology of the disease.
I Quincke und Roos: Berl. klin. Wochenschr., 1893. 2 Hlava: Centralbl. fur Bacteriologie, 1887.
3 Massaiutin: Ibid. 4 Nasse: Deutsche med. Wochenschr.. 1891.
5 Osier: Bulletin of the Johns Hopkins Hospital, 1890.
6 Stengel: Medical News, November 15th, 1890.
7 Musser: University Med. Magazine, December, 1890. 8 Eichberg: Medical News, August 23d, 1891. 9 Stockton: International Clinics, 1894, i.
10 W. J. Councilman and H. A. Lafleur: " Amoebic Dysentery." Johns Hopkins Hospital Reports, vol. ii., Nos. 7-9. 1891, p. 395.
II K. F. Harris: "Amoebic Dysenteny." American Journal of the Medical Sciences, 1898, p. 384.
12 Schuberg: Centralbl. fur Bakteriologie. 1893.
It is generally believed that the amoebae enter the system along with the food or drink. Sodre believes that they can be taken in with the air. Certain waters, however, apparently constitute the principal means of propagation of these amoebae. Thus, Barthelemy 1 relates that the troops when operating on the shore of the Oueme, whose clear running water was filtered in Chamberland filters before being used, were in good health and free from dysentery; when, however, the army moved away from the Oueme in the direction of Abomey they were compelled to use unfiltered swampy water. From that moment dysentery made its appearance. Fitz and Gerry 2 described a case of dysentery with the presence of amoebae in the stools and found the same micro-organisms in a cistern, the water of which the patients constantly used.
Age does not seem to have any influence upon the disease. Statistically a greater number of cases is found among adults, as these are more exposed to the morbific causes. Both sexes are equally predisposed to dysentery, and no race enjoys immunity from it. One attack does not confer immunity against others. Persons who suffer from want of food or who live on food of bad quality are most liable to contract the disease. Harris says: "Dysentery is a disease pre-eminently of the poor, and is almost always associated with filth, bad hygienic surroundings, and lack of proper food." This statement, however, is somewhat too categorical, and I fully agree with Sodre, who remarks that dysentery is observed also in persons of the wealthier class, who live on the best food and are surrounded with every comfort. Nevertheless, it must be admitted that it is most frequent among the poor, and chiefly among people who live under bad hygienic conditions.
1 Barthelemy . " Medical Report of the War of Dahomey " 2 Fitz and Gerry: Cited after Sodre, loc. cit.
Morbid Anatomy
In acute dysentery the large intestine is almost always found in a thickened condition. This thickening involves all the intestinal coats, but is most marked in the snbmucosa. Sometimes the latter layer alone is involved. The mucosa, when washed with water, presents a bright red, at some places dark red color. The folds of the mucosa are much more voluminous than normally, and thus present considerable prominences. Small red nodules of various size are also seen scattered over the* mucous membrane. Besides these nodules more or less numerous ulcers are found. These vary greatly in size (from a pinhead to two inches long) and also in depth, some being superficial, others quite deep. The ulcers are situated chiefly on the folds of the mucosa. Ordinarily they are oblong and lie transversely to the long axis of the bowel. Sometimes they are circular, sinuous, or irregular.
Councilman and Lafleur have described on the surface of the mucosa sharply outlined projecting nodular thickenings, in which are observed cavities filled with a gelatinous mass communicating with the surface of the mucous membrane by small openings, frequently not larger than the head of a pin. These writers have also pointed out as characteristic of the dysenteric ulcers their undermined edges. The disease process in dysentery, according to Councilman and Lafleur, is essentially one of advancing infiltration and softening of the submucous and intermuscular tissue with subsequent necrosis of the overlying tissue. The amoebae reach the submucosa without injuring the mucous membrane. Here the essential changes are first produced, and the mucous membrane is interfered with later. The mucosa becomes oedematous and ruptures after a while, forming an ulcer.
Harris described two anatomical forms of ulcers found in dysentery. In the first form, which is encountered most frequently and can be considered as the typical intestinal lesion of the disease, changes in the submucosa may be traced in advance of the surface ulceration for quite a distance, thus undermining the comparatively healthy mucosa above. In the second form the ulcers increase in size by gradual softening and breaking down at the surface, never by necrosis and sloughing of the underlying tissue. Ulcers of the second category occasionally do not penetrate deeper than half -way through the mucosa. Generally they extend into the submucosa. They never contain amoebae.
The lesions described are usually found throughout the entire large bowel, but as a rule they do not extend beyond the ileocaecal valve. In a comparatively small number of cases the small intestine is also involved, principally the ileum.
In some instances gangrene of the intestine is found. Many authors even describe a gangrenous form of dysentery. Sodre, however, does not regard the gangrene as a lesion brought on by the amoebae dysenteriae, but by the action of bacteria foreign to the dysenteric process. According to this author gangrene is a complication of dysentery, but not a specific lesion. In this complicated form, besides the ulcers described above, there exist others of a gangrenous character. The gangrenous process may also extend beyond the ulcers. On the brownish-red mucosa gangrenous patches of a dark color and of various size are seen. In this condition the mucosa may be detached over a considerable area and eliminated with the dejections.
In chronic dysentery the intestine is pale with slate colored spots. Its walls are thickened. The mucosa presents a pale rosy or slate color. Ulcers in different stages of development are encountered. Often the ulcers occur in groups separated from each other by more or less extensive healthy areas of intestine. Sometimes in certain portions of the intestines the ulcers become confluent. Dysenteric ulcers may be round, elliptical, or serpentine in form and usually have thickened and callous edges. In the neighborhood of the ulcers, there is no hyperaemia or cedema, although an increase of fibrous tissue is noted. Undermined ulcers undergoing a process of repair are also found. The mucosa glands are found dilated and filled with mucus. In some places glandular cysts of considerable size are encountered, in others the glands have almost disappeared, and only traces of them are left. The mucosa is thickened and filled with round cells. The submucosa is likewise thickened and in some places cedematous.
Dense fibrous tissue is found almost all over in this layer, predominating, however, at the location of the cicatrices and of ulcers in the process of repair.
In both the chronic and the acute form of dysentery, but principally in the latter, besides the lesion of the intestine- described above, the liver is frequently found diseased. In dysentery complicated with gangrene this organ is usually greatly increased in volume, tumefied, soft, and friable. The cross-section presents a dark color interspersed with yellowish spots. The latter are usually somewhat raised above the surface. On microscopical examination the hepatic cells show a large amount of fat; besides, small round abscesses are found around the capillaries, which are most probably due to emboli.
Aside from these very small pus collections of pyaemic origin, other abscesses are found which differ from these by their size and the nature of their contents. They are the so-called dysenteric abscesses of the liver, and are most often encountered in acute dysentery without gangrene. The dysenteric abscesses vary greatly in size from a few lines to several inches. They are situated chiefly in the right lobe of the liver near the surface. Often several are found together. The contents of these abscesses vary greatly. In the most recent, the abscess does not empty itself on section. A small amount of glairy, semi-transparent fluid exudes and leaves behind an irregular spongelike mass, the fluid being apparently held in the meshes. In the older abscesses the contents are more fluid, the latter having a greenish opaque color. In these are suspended some solid masses of tissue. In some instances the contents are brownish or streaked with brownish-red from admixture of blood. Microscopical examination of the contents of the abscesses reveals the presence of a few pus cells, a large quantity of fatty granules, necrotic hepatic cells, a few blood corpuscles, a great number of amoebae (see Fig. 28), and sometimes micrococci and bacilli.
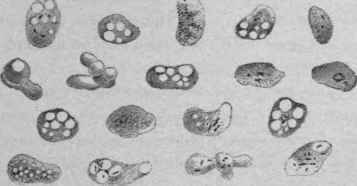
Fig. 28. - Amoebae from an Abscess of the Liver. X 750. (Sodre)
According to Councilman and Lafleur, there is no definite abscess-wall, the liver tissue passes gradually into the abscess, and the contour of the edge is very irregular, sometimes extending into the liver for a distance of several nodules. The abscess may penetrate the capsule of the liver and either open externally or it may burst into some of the adjacent organs, as, for instance, the lungs, the stomach, the intestines, or the peritoneal cavity. Most often, however, it bursts into the lungs.
Continue to:


