Auxiliary Therapy
Description
This section is from the book "Progress Against Cancer", by National Advisory Cancer Council. Also at Amazon: Progress Against Cancer.
Auxiliary Therapy
Auxiliary, or supportive, therapy to overcome problems resulting from the disease process or drug side effects has been developed along with the drug treatment techniques. Results have been particularly effective in patients with acute leukemia, whose most serious complications are hemorrhage and infection. Hemorrhage stems from a shortage of blood platelets, and infection from a shortage of granulocytes (white cells) in the blood (page 38).
Adaptation of a plasmapheresis (plasma-removing) technique has solved the problem of obtaining the fresh platelets needed in large numbers for transfusion into patients to prevent or stop hemorrhage. Platelets and plasma are removed from whole blood and the red cells promptly returned to the donor in one continuous operation. The advantage of this procedure is that it permits donors to give platelets as often as twice a week for periods up to three months; by conventional procedures, they can give blood only once every six to eight weeks. A single adult donor can provide the major portion of the platelets required by a child with leukemia.
The use of platelet transfusions has resulted in substantial reduction in the frequency of death from hemorrhage, and has not only kept patients alive until drugs could take effect but permitted increased opportunity for use of effective drugs that depress platelet production. Frequently, in the major leukemia centers, transfusions are given as a preventive measure whenever the platelet count falls to dangerously low levels.
The transfusion of white blood cells for treatment of some infections is a more difficult problem. Antibiotics are also employed for this purpose, but in the absence of competent white cells they are often not effective.
Normal donors have few circulating white cells compared with red cells and platelets. However, the National Cancer Institute is sponsoring the development of a continuous flow blood-cell separator which is expected to produce adequate amounts of these white blood cells from normal donors. Essentially the instrument utilizes a centrifuge that operates on the principle that the blood components have different densities. Blood is separated into three main fractionsplasma, red blood cells, and white blood cells. The blood-cell separator is designed to operate on a continuous flow basis, and when fully developed will draw a donor's blood, remove white cells, and return the other elements to the donor. The blood will flow in a closed system from a vein in one arm of the donor, through the separator, to a vein in the other arm. No more than one pint of donor's blood will be outside his body at a time. In principle, this procedure would make it possible to obtain from the blood of a single donor the granulocytes needed for one transfusion. At present more than 30 normal donors are required to obtain an adequate number of granulocytes.

The blood cell separator, shown here, is being developed to make available for transfusion into leukemia patients adequate amounts of a type of white blood cell that combats infection. When fully developed, the separator will operate on a continuous flow basis, and will draw a donor's blood, centrifuge it to remove the white cells, and return the other blood elements to him.
In tests of the blood-cell separator on a continuous flow basis, good yields of granulocytes have been obtained from normal human volunteers. These white cells have been found viable and suitable for transfusion into patients. Preliminary results indicate that they are effective in controlling infection in a few cancer patients.
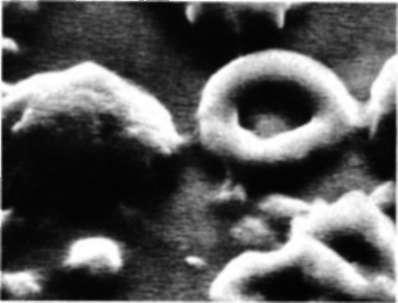
These blood cells were magnified 6,000 times by a scanning electron microscope. Large, fluffy mound is white blood cell: red cell appears doughnut-shaped; small sphere is a blood platelet.
Another approach is the development of relatively germfree treatment areas for protection of patients from infections. A continuing study of the "Life Island," a plastic bubble that encloses a bed, has shown that the incidence of infection is reduced in patients within the germfree environment of the isolator. It has been possible to maintain a patient for long periods of at least three months in this environment. Whether drug toxicity is reduced remains to be established, but the impression thus far is that toxicity is somewhat less even when large doses of drugs are used. Maintenance of patients within the plastic bubble is a demanding, elaborate procedure for both the patient and the hospital staff, and it is difficult to assess the role of this technique at present.

A plastic bubble provides a relatively germfree environment for the patient. Its use with cancer patients has reduced the risk of infection during intensive drug treatment.
To enlarge on the idea of the plastic isolator, development of laminar-flow rooms is in progress. In such rooms it is expected that patients will be protected from infections by a controlled flow of recirculating, filtered air. Visitors entering downwind will not infect the patient with bacteria because contaminated air is blown into filters and rendered germfree before it is recirculated to him. Too, the psychological disadvantage of confinement in the plastic bubble is overcome by this technique.
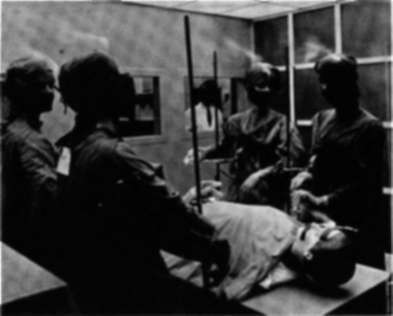
The "laminar flow" system of air supply, illustrated here, is designed to reduce bacterial levels in hospital rooms. Air passes through a wall of high-efficiency filters, flows horizontally across the room and up to ceiling vents, and is refiltered and recirculated. The scientist in the background observes air flow patterns from smoke devices on mannequins' heads.
An even newer concept would employ a portable laminar-flow unit to transform an ordinary hospital room into a "protective environment" for virtually germfree care, without the extensive building modifications required to install a laminar-flow room.
Continue to:


