Infarction
Description
This section is from the book "A Manual Of Pathology", by Guthrie McConnell. Also available from Amazon: A Manual Of Pathology.
Infarction
An infarct is the area of degeneration and inflammation produced by embolism in an end-artery or where there is an absence of adequate anastomosis. The act of obstruction constitutes infarction, and must be sufficiently sudden to prevent the establishment of any collateral circulation.
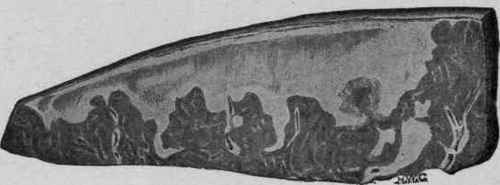
Fig. 5. - Part of Spleen the Seat of Multiple Anemic Infarcts (Coplin).
Infarcts occur chiefly in the so-called end-arteries of Cohn-heim - those that terminate in veins or capillaries without anastomosis with an artery. They are found particularly in the kidney, spleen, base of the brain and lungs, and sometimes in the heart.
The varieties of infarcts are: (I) Anemic or white; (2) hemorrhagic or red.
The anemic occur more commonly in solid organs, such as the kidney; the hemorrhagic, in organs whose structure is loose, as the lungs. The spleen may be the seat of either form.
An anemic infarct is one in which there is an absence of blood. The essential cause of this form is probably the relatively rapid death of the tissues with coagulation before the capillary anastomoses have widened sufficiently to cause hemorrhage. There is usually a narrow hemorrhagic zone surrounding the lesion.
In this type there is probably present a secondary blood-supply sufficient to prevent the occurrence of coagulation necrosis.
A hemorrhagic one is where the obstructed area is full of blood. It may be the result of a back flow of blood from the veins (Cohnheim's theory) or from free capillary anastomosis. The latter would be particularly apt to occur when the local or general blood-pressure was previously elevated; or when the lodgment of an embolus caused a reflex contraction of the surrounding vessels and thus brought about an overflow of blood into the occluded area through the capillary anastomoses. Another theory is that the blood does not escape until there has been some degeneration of the vessel walls.
When the blood is cut off a conical shaped area of tissue is deprived of nutrition. As a result, necrosis soon starts in. The apex of this area is directed toward the interior of the organ, the base to the external surface. The base will be swollen and project above the surface of the surrounding tissues.
The infarct is, as a rule, firmer than the rest of the organ, except when it occurs in the central nervous system, where it is usually softer; the firmness depending upon the amount of coagulable material present.
Infarctions of the lung are unusual, as in that organ the capillaries are comparatively large, and the anastomosis between the pulmonary and bronchial arteries may be sufficient to prevent necrosis. To have infarcts occur within the lung, that organ must have been the seat of previous disease.
Results
Infarction is always accompanied by necrosis and fatty degeneration, (I) The tissue may be restored by absorption and by collateral circulation. (2) It may be replaced by connective tissue with the formation of a scar. (3) It may become encapsulated. (4) Very rarely an infarct may undergo liquefaction necrosis with cyst formation, particularly in the brain.
Continue to:


